The weekend before we were scheduled to leave for a week-long beach vacation, I noticed that Murphy was showing symptoms of her cancer growing or spreading. The mast cell tumor on her right side had been previously flat and flush with the rest of her skin, just a different color. It was now beginning to look raised and becoming a little darker and irritated. I had carefully been observing every time she urinated outside, since any change in frequency, width of the stream, or inability to produce a steady stream could signal pressure on her bladder from the lymph node near her spine, the very same lymph node that was removed, regrew, and radiated a month or so later. Since she began radiation in May, she had been taking Palladia, the first FDA-approved chemotherapy specifically for dogs, three days a week. I noticed over the previous two weekends, that the tumor on her side grew a little bit over the weekend breaks from the chemo. I also noticed her stream was getting narrower. Which is why I scheduled her ultrasound for the Thursday before we left for vacation. She wasn’t due for another 10 days, but she was showing just the slightest signs of the cancer affecting her again. We’d been through this before; Mike and I were now aware of the tiniest signs that, when ignored, led to disastrous results. The ultrasound showed that the lymph node was larger than we had hoped it would be, though not as big as it was prior to radiation. The doctor and I agreed that we should increase her Palladia dosage. She may experience side effects, but this was our best shot to get this thing under control. The increased dose had to be shipped from another animal hospital, so she’d receive two more pills at her current dose, and hopefully be able to take the new dose starting the following Wednesday while we were on vacation. This was our best chance of getting ahead of this thing before it took over her body again. We both realized that if this cancer did take over again, we would be in a tight spot. We were running out of both time and options that she could physically handle.
About a month before we left for vacation, I told MIke that I had a bad feeling. Our vacation was exactly two months post-radiation. The oncologist gave us a prognosis of two months of quality-living for Murphy with radiation, maybe more. We were foolishly optimistic, and believed there would be many many more. When I told Mike about my bad feeling, he told me not to say that, or not to think that way. But I couldn’t shake it. This is why I was so observant, this is why I scheduled the ultrasound ten days early. I was trying to be proactive and detect changes before they became unmanageable.
Murphy’s medicine didn’t arrive on Wednesday like it was supposed to, meaning another day at the lower dose. I was stressed because my cell phone had poor reception, so I couldn’t call the vet and was relying on text messages from my mom to get info on the drug shipment. My whole family was leaving for a cruise the next day, unreachable by cell phone until Monday. Our pups were staying with my in-laws, but they aren’t exactly dog people. They love our pups as much as they can, and they respect the way we love our pups, but I didn’t feel comfortable asking them to deal with the vet. When we checked in with Murf, she was doing Ok. She was taking a long time to go potty, but she was still making. She wasn’t bloated. She had a lot of energy, and was eating and drinking normally.
Thursday night, my father-in-law called Mike. Within a day, she had gone from ok, to miserable. She was tinkling all over the garage, but she couldn’t make when she wanted to, meaning that her bladder was likely so full, she was urinating by accident. She couldn’t control what came out and when. She was also refusing food. That had never happened before. Murphy was always hungry. She never refused food. This was bad news. In exactly a week from the ultrasound, the lymph node had grown from larger than desirable, but not intrusive, to out of control, affecting her in a very negative way. It was compressing her bladder, just like it had back in February and again in April. We knew what this meant, but we were in Florida. We needed to get home to her before we could make any logical decisions. After a pretty intense conversation with the night-shift emergency vet, and a ton of tears, we agreed that we would cut vacation short by one night. Mike’s dad would bring Murf in first thing Friday morning so they could place a urinary catheter and make her comfortable. She would stay overnight, and then we would drive out Friday night, when there was less traffic, allowing us to be with her Saturday morning.
Meanwhile, her higher-does chemo arrived on Friday, and she was given the pill that afternoon. I was furious that the shipment arrived two days late, essentially losing time to effectively treat this growing cancer. I was furious that we did everything we could to be proactive about her treatment, and yet nothing could be done. We knew how quickly this cancer grew and wreaked havoc on her body, so we did our best to convey the urgency of the situation to any and everyone we spoke with at the vet clinic. At the time, I felt like they weren’t taking me seriously. With a little distance from the situation, perhaps they were taking me seriously, but also, in their vast experience, knew what we were dealing with, and how little we could truly do to stop it. I’ll never know.
After an emotional Thursday night and a low-key rainy day Friday, we left Florida around 9PM, and arrived home around 2AM. Malcolm and I woke up around 7AM, and went to visit Murphy at the animal hospital around 8:30. She looked tired. For the first time ever, throughout this entire disease, she looked tired. I don’t mean sleepy. I mean tired of fighting. She wasn’t nervous, never tried to bark or growl, wasn’t shaking from nerves or excitement, none of her old habits of her past hospital stays were present. She just looked simply tired. She was passing a lot of blood through her urinary catheter, which probably made her even more tired.

The vet, Dr Brown, was so kind. She explained everything to me and allowed me to visit with Murf as long as I wanted to, even with Malcolm banging toys and opening cabinets and generally making a ruckus. She didn’t mind. Our plan was to get to Monday. We knew that Murphy was at a very grave and critical point, but our normal vet, Dr. Crawford, had been out since Wednesday. We did not feel comfortable taking any drastic steps in Murphy’s treatment without Dr. Crawford’s advice. She knew what Murf had been through and what she could handle. So that was our plan. We could come and visit as often as we’d like, but Murf needed to stay in for monitoring until at least Monday.
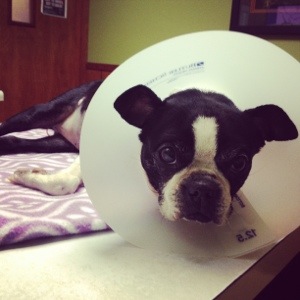
When the three of us visited Murf on Saturday night, she was eating a little bit, finally. They gave her some rotisserie chicken, plus she was taking treats from our hands. She looked a little more tired than she had that morning. Perhaps it was the stress of being in the hospital. Perhaps not. She did seem to perk up just being with us. Or was that my imagination? She ate treats from our hands and allowed us to cuddle and kiss her as much as that stupid e-collar would allow. The e-collar was to prevent her from pulling out her catheter. It was an emotional visit, but we stuck with the plan. Get to Monday. Dr. Sarah answered all of our questions about Murphy’s progress, what our options were, and whether these options were good options. She was patient and gentle with us. We were beginning to have some difficult conversations, and she was so careful with her words, so kind in her delivery. We were disappointed with how little Murphy was progressing, but still, unless absolutely necessary, no decisions would be made before Monday.

Sunday morning was the baptism of Mike’s new godchild, and it was an absolutely beautiful day. A celebration of life, love, and family, both physical and spiritual. Murphy stayed in the back of my mind, and I prayed for strength and courage for both Mike and me, and for Murphy. When we visited her that night, she looked weaker, still. Even more tired than the previous evening. She was losing strength and muscle tone in her legs. They had connected her to an IV for fluids, because she wasn’t drinking water, but was having diarrhea. This was so unlike her. At home, she drank so much water, she could drink the whole bowl and still want more. We knew things were not going in our favor, but still, “Get to Monday” was the plan. We also noticed some pretty severe bruising on her abdomen. The doctors hadn’t even noticed it. It seemed pretty new. We didn’t see it on Saturday. Dr. Brown believed it was a platelet issue. The way to solve it was a blood transfusion. She’d already had two before, so they’d have to cross-match, whatever that means, I guess making it more complex. We were nervous about a transfusion. Could she handle it? Was it truly necessary? Blood work showed that she didn’t yet need a transfusion, so again, back with the plan – get to Monday. Continue to monitor her blood, urine, hydration, appetite, and now bruising. We couldn’t wait to get Dr. Crawford involved and get some answers from the oncologist too.